Obsessive-compulsive disorder (OCD) is an anxiety-based mental health condition that affects roughly 1.2% of the general population. Its main symptoms are adverse, obsessive and intrusive thoughts, together with repetitive, compulsive behavior, both of which end up adding to the patient’s stress level.
Due to a rise in awareness of this debilitating mental health condition, OCD therapy is being studied more than ever before. This includes both first-time patients and those found to be resistant to first-line treatments, who are also known as treatment-resistant patients. It is for these patients that further treatments that go beyond first-line OCD treatments, such as SSRI medication and cognitive-behavioral therapy (CBT), may offer long-awaited relief.
Additional Therapies for Those Who Need Them
These days, treatment-resistant patients are looking beyond the most common available therapies, in an effort to find one that works for them. That said, it remains unclear how many people are even considered “treatment-resistant”: OCD research continues to struggle to define who, exactly, falls under the definition for “treatment-resistant” patients with OCD, and as a result have trouble calculating how many people have benefited from additional treatment options.
Generally speaking, treatment resistance describes patients who have not significantly benefited from SSRIs (a mood-balancing medication that maintains higher levels of active serotonin), or CBT (a form of goal-oriented psychotherapy). That said, defining the cutoff line for those who have benefited from first-line treatments and those who have not remains somewhat murky. A comprehensive meta-analysis from 2002 attempted to answer this dilemma, determining that 40%-50% of patients with OCD are considered treatment-resistant. A more recent study from 2015 found that 42% of all patients with an OCD diagnosis are treatment-resistant.
So what treatments are available for treatment-resistant patients, who have yet to find real relief from first-line, go-to forms of therapy? The following list groups together several additional options, which different empirical studies have found to offer significant results:
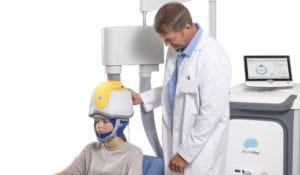
Deep Transcranial Magnetic Stimulation (Deep TMS): Deep TMS utilizes magnetic fields to safely and effectively regulate the neural activity of brain structures found to be associated with OCD. The only non-invasive medical device to be FDA-cleared to treat OCD, Deep TMS does not require any anesthesia and can be incorporated into the patient’s daily routine. Numerous studies have shown this treatment to effectively alleviate symptoms of OCD, thereby providing patients with a significantly better quality of life.
Clomipramine: Clomipramine is a tricyclic medication that keeps the neurotransmitters serotonin and norepinephrine active for a longer period of time. Since it effectively influences serotonin, clomipramine manages to achieve a similar level of symptom relief to that of first-line treatment of SSRI medication. However, while it has been found to be as effective as SSRIs, clomipramine’s more severe side effects make it more difficult for many patients to continue taking. Another cause for concern is that clomipramine (again, similarly to SSRIs) usually necessitates higher dosage to effectively treat OCD, than it would to effectively treat major depressive disorder (MDD).
D-cycloserine: Originally used as an antibiotic for tuberculosis, D-cycloserine has been found to effectively treat anxiety-based mental disorders. As a partial binding agent with the neurotransmitter glutamate, D-cycloserine is able to affect extinction learning: to put it simply, research has shown that D-cycloserine can help “unlearn” connections our mind makes, between stimuli and the anxiety they cause within an OCD context. As a result, introducing D-cycloserine during the exposure stage of first-line CBT treatment can prevent the patient obsessed with illness and contamination from experiencing anxiety when confronted with a dirty dishrag. Though initial results have been promising, D-cycloserine’s efficacy still needs to be substantiated through additional studies, before it can be considered a widely-effective form of OCD treatment.
Saffron: In addition to adding flavor, the exotic and high-end spice has also been linked to reduced OCD symptom severity. In fact, a recent study found it to be as effective with mild-to-moderate OCD as the SSRI fluvoxamine, which has been FDA-approved to treat OCD since 1994.
Passionflower Extract: The flowering passion fruit plant has first-generationly been used by Native American tribes as a calming agent. Initial clinical trials have confirmed that that passionflower extract has anxiolytic (anti-anxiety) properties, which can help reduce stress in cases of OCD.
N-acetylcysteine (N-AC): N-AC is an antioxidant derived from the amino acid cysteine. While it is more commonly used to counter Tylenol poisoning, it also affects the neurotransmitter glutamate, which has been linked to OCD. The current research on N-AC shows some potential, particularly when administered in tandem with SSRI or tricyclic medication. However, as much of N-AC research is based on individual case studies, and since there is still insufficient evidence of its effects as a monotherapy for OCD, further research is needed to determine its efficacy and tolerance.