With the increased focus on OCD in recent years and a growing number of treatments for this condition, it is important to understand the different factors that influence it and its central defining characteristics. For this reason, to truly understand OCD, you have to look at the family of mental health conditions that it branches out of—anxiety.
OCD and anxiety are considered groups of mental health conditions that relate to each other in terms of shared symptoms, possible comorbidity and the detrimental effect they can have on the quality of life. In fact, perhaps the most debilitating OCD symptom is the anxiety it induces in the individual experiencing it.
Despite their commonalities, though, OCD and anxiety are currently classified separately and can respond to different treatment options with their own level of success. As such, it is important to understand their own unique and common characteristics, and how to best approach each of them.
Anxiety has long been a key targeted condition in the battle for greater mental health. Described as excessive, adverse anticipation of a future threat, anxiety is considered a disorder due to its over-responsiveness to an intimidating thought, stimulation or scenario.
Anxiety shares certain traits with fear while differing in other regards. While fear is an adverse, emotional reaction to an actual and real threat, anxiety is a similar reaction to the possibility of a threat. Additionally, while fear is considered a proportional response to a present threat, fear (or temporary anxiety) tends to pass, while anxiety disorder is defined by its persistent nature.
Anxiety disorders are fairly common, with an estimated 19.1% of US adults facing some kind of anxiety disorder, and 31.1% of US adults facing one at some point during their lives. It should also be noted that anxiety disorders are diagnosed more commonly among females than males, with a 2:1 ratio.
The DSM’s current edition, the DSM-V, was released in 2013 and is the main mental health diagnostic manual used within the US. It describes a number of disorders within the anxiety family:
Obsessive-compulsive disorder, or OCD, is an anxiety-based mental health condition that includes anxiety-inducing thoughts, actions, or both. In OCD, ruminative and stressful thoughts cause the individual to carry out repetitive behavior intended to calm down the anxiety they are experiencing. However, rather than helping assuage their distressing thoughts, OCD behavior contributes to their rising anxiety, creating a cycle that is detrimental to their own well-being, relationships to others, and general quality of life.
It should also be mentioned that OCD is currently a part of a number of OCD-related disorders. This spectrum of conditions includes trichotillomania (hair pulling), hoarding, excoriation (skin picking), and body dysmorphic disorder (a preoccupation with one or more perceived defects in physical appearance).
 Obsessive Thoughts: OCD is in essence an overactive defense mechanism that causes a disruption to an individual’s mental health system. This is initially manifested through ruminative, obsessive thoughts that introduce a great deal of distress and anxiety into their system.
Obsessive Thoughts: OCD is in essence an overactive defense mechanism that causes a disruption to an individual’s mental health system. This is initially manifested through ruminative, obsessive thoughts that introduce a great deal of distress and anxiety into their system.
The following four categories are considered to be the most common themes of OCD-related thoughts, beliefs, urges or images. They can appear individually or in combination with one another:
These thoughts and beliefs are experienced in OCD as intrusive, unwanted and disturbing. They can disrupt an individual’s routine and cause them a significant amount of distress, worry, and frustration.
Apart from the type of content that grow into OCD-related obsessions, OCD is defined by the level of insight an individual has into their condition. This ranges from a good level of insight (recognizing they are facing a mental difficulty) to no insight at all (an inability to acknowledge it). Many patients may simply rationalize their OCD symptoms as personality quirks that are not symptoms of a more substantial mental health condition.
Compulsive Behaviors: In addition to feeling attacked by their own obsessive thoughts, individuals facing OCD may develop compulsive mechanisms of behavior, as a way to calm the severe anxiety they experience. These mechanisms, however, can end up causing them further anxiety as well, while also disturbing the individual’s physical, mental, emotional and social well-being.
OCD-related compulsive behaviors can be quite diverse, ranging from repetitive hand washing, checking and rechecking that all electric and devices in the house are safely turned off, losing hours and days to meticulously arranging the items on your desk in a symmetric layout, or repeating a certain action in an attempt to ward off an alarming thought.
Though such compulsive actions are carried out as a way to satisfy an obsessive thought, eventually the compulsive behavior begins feeding the obsession: for example, an individual who had originally washed their hands to calm their contamination anxiety, will likely in time continue with their washing ritual for longer and longer periods of time, without finding relief from their lingering thoughts that maybe this time they had nevertheless caught an infection.
Prevalence: An estimated 1.2% of US adults are facing OCD, with a lifetime prevalence of 2.3%. The DSM goes on to state that females tend to suffer from OCD at a slightly higher rate than males. OCD tends to manifest during early adolescence and often goes undiagnosed for over a decade.
Unlike the DSM’s previous edition (the DSM-IV), the DSM-V does not include OCD as part of the anxiety family. However, it does mention the relatedness between anxiety and OCD, noting their shared history and anxiety-centered symptomatology.
The World Health Organization’s (WHO) global diagnostic manual is called the ICD, and its latest English edition, the ICD-10, was published in 2016. While it cites OCD separately from anxiety disorders, it does include both under the larger “neurotic, stress-related, and somatoform disorders” disorders umbrella.
Both the DSM and ICD eventually moved OCD out of the anxiety family and began viewing it as its own group of disorders. This shared development, however, was less than intuitive: in addition to anxiety literally being a key factor of OCD, the prevalence of OCD is considerably lower than specific anxiety disorders such as social anxiety disorder (7% among the US adult population), or general anxiety disorder (2.9%). So why has OCD been singled out? The answer seems to be a mix between two main factors: clinical research and marketing.
Clinical studies from the past several years have outlined the ways OCD differs from other anxiety-based disorders, while backing different theories as to why this is the case. Several studies have concluded that OCD-related disorders share familial and genetic factors, relevant neurotransmitter/peptide systems, neurocircuitry, phenomenology, comorbidity, and treatment responses. Abnormalities in the anterior cingulate cortex and frontal striatal pathways in particular have been shown to be associated with OCD.
Concurrently, the Executive Functioning Hypothesis posits that a disturbance in an individual’s self-regulatory abilities causes OCD, while other anxiety-based disorders are mainly associated with emotional processing.
Further neuroscience and mental health research is ongoing to clarify the relationship and differences between OCD and Anxiety.
While some of OCD’s prominence is due to advances in research, some of it is due to what the general public understands OCD to be, whether correctly or not.
Many entertainment articles have pushed forward a less clinical take on OCD, so that many positive qualities, such as cleanliness, good organizational skills and efficiency, have been dubbed “OCD traits”. Such generalizations run the risk of conflating a personal tendency with a potentially debilitating mental health disorder.
While downplaying the more severe aspects of OCD can at times make light of a serious disorder and create a fair amount of confusion over who actually suffers from OCD, sometimes popular articles can get it right. The extra attention OCD is receiving also helps fight the stigma around this disorder, and creates an increased desire to aid and assist those battling it.
With OCD now presented on its own in both of the DSM and ICD, a higher level of visibility has been awarded to this disorder. Its new level of prominence has become clear through the surging number of studies dedicated to OCD research, the introduction of serotonin-focused medications shown to treat OCD, and a rise in media coverage, all highlighting a greater public and professional increase in this condition.
Several treatments for OCD are now available as means to address OCD and its symptoms:
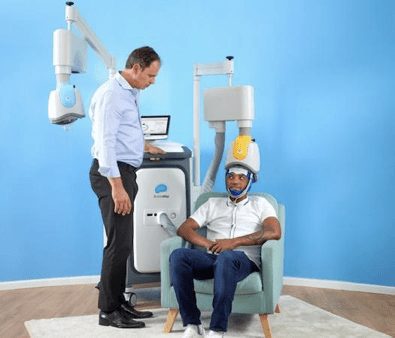 Deep TMS™: The only non-invasive medical device FDA-cleared to treat OCD, Deep Transcranial Magnetic Stimulation (Deep TMS) utilizes magnetic fields to safely regulate the neural activity of brain structures found to be related to OCD. Its stimulation of the medial prefrontal cortex and anterior cingulate cortex was found to effectively alleviate symptoms of OCD in a multicenter, sham-controlled study published by the American Journal of Psychiatry in 2019.
Deep TMS™: The only non-invasive medical device FDA-cleared to treat OCD, Deep Transcranial Magnetic Stimulation (Deep TMS) utilizes magnetic fields to safely regulate the neural activity of brain structures found to be related to OCD. Its stimulation of the medial prefrontal cortex and anterior cingulate cortex was found to effectively alleviate symptoms of OCD in a multicenter, sham-controlled study published by the American Journal of Psychiatry in 2019.
Cognitive Behavioral Therapy: CBT is a form of psychotherapy that is often used to treat OCD. The treatment focuses the thoughts, feelings, behaviors and physical reactions that arise from the individual’s OCD, helping them become less anxious in the process. Several types of CBT have been found to be effective in treating OCD, in particular acceptance and commitment therapy (ACT). ACT helps patients experience psychological openness and flexibility in as they react to intrusive, obsessive thoughts, in addition to building their commitment to their own behavioral change.
Exposure and response prevention therapy: (ERP) has been shown to effectively treat OCD. In ERP, the patient is gradually exposed to their source of anxiety, with the therapist accompanying them along the process, encouraging them to avoid acting out of compulsion.
Psychopharmacology: There are several types of psychiatric medications prescribed for OCD, with a number of antidepressants FDA-approved to treat the disorder. While many patients find medication to be helpful in alleviating their OCD symptoms, they may also include possible, adverse side effects.
Psychodynamics: Another form of psychotherapy sometimes considered for OCD treatment is psychodynamic therapy. It focuses on the interplay between formative relationships and life events, needs and desires, theoretical mental structures and personality traits, as patient and therapist work to understand what may have caused the development of OCD. Together, they set out to deconstruct the more rigid, maladaptive patterns the patient has linked to the disorder, as they begin to consider more beneficial alternatives.
We urge you to consult your mental health provider regarding the type of treatment that might be right for you.