From research to news coverage to observations in the field, symptoms of depression have been shown to be on the rise. As a result, many individuals facing this condition oscillate between medication vs. TMS therapy for depression in an attempt to figure out which treatment course could best alleviate the symptoms of this persistent disorder. Read on to learn about their different attributes.
Psychopharmacology has long been considered a go-to treatment for depression. This mood disorder, known as major depressive disorder (or MDD), is ranked among the most prevalent mental health disorders in the world. This disorder is marked by feelings of emptiness, sadness, a lack of joy, hopelessness and difficulty concentrating. As a result, proven effective treatments for this condition are in high demand, with many physicians prescribing some form of antidepressant for patients struggling with this disorder.

A number of antidepressant families have been FDA-approved to treat MDD. Selective serotonin reuptake inhibitors (SSRIs) and serotonin-norepinephrine reuptake inhibitors (SNRIs) are usually prescribed as first-line treatments due to their efficacy and safety Tricyclic antidepressants (TCAs), however, are considered a second-line form of treatment which while effective, is less frequently prescribed due to tolerability issues.
SSRIs
Widely available since the mid-1980s, selective serotonin reuptake inhibitors work by preventing the reabsorption of the neurotransmitter serotonin into the neuron’s synaptic cleft, thereby extending the neurotransmitter’s period of efficacy.
SNRIs
Serotonin-norepinephrine reuptake inhibitors have been publicly available since the mid-1990s, combining some of the benefits of tricyclics and SSRIs that came before them, meaning SNRI’s keep both norepinephrine and serotonin active for longer.
TCAs
Tricyclics block the reabsorption of the neurotransmitter norepinephrine, which has also been associated with mood disorders. They have been available since the late 1950s and early ‘60s, and were part of a larger move in depression research to achieve remission by focusing on a specific neurotransmitter’s connections.
Transcranial magnetic stimulation utilizes a series of electromagnetic pulses, which are broadcast through a cranial apparatus to regulate the brain’s neural activity. TMS for depression treatment has been shown to help alleviate the adverse symptoms of a number of mental health conditions, and primarily those of depression. It is safe, non-invasive, and does not require anesthesia.

There are currently two kinds of TMS available on the market: First-Generation TMS and Deep TMS.
First-Generation TMS
first-generation transcranial magnetic stimulation has been available to the general public since 1985, and as a treatment for depression since 2008. First-Generation TMS uses a handheld, figure-8-shaped device to send out its electromagnetic pulses and has been FDA-cleared to treat depression.
Deep TMS
Deep Transcranial Magnetic Stimulation also utilizes magnetic pulses to regulate the neural activity in brain structures associated with depression.
Unlike First-Generation TMS, Deep TMS uses a cushioned helmet that holds its patented H-coil technology. Its apparatus and technology allow it to reach deeper brain regions directly in addition to reaching wider swaths of the brain with each pulse.
Deep TMS has been FDA cleared to treat depression since 2013.
Both antidepressant medication and TMS have been shown to safely offer symptom relief to those battling depression. Both forms of treatment also come with their own possible side effects.
The possible side effects from the above-mentioned medications vary from patient to patient. The following represent some of the more commonly cited side effects for three groups of antidepressants:
SSRI Side Effects
SSRI side effects commonly include weight gain and sexual dysfunction. Along with sleep disturbance, the above mentioned are considered the more common long-term side effects of this group of medications. With that said, SSRI side effects usually lessen or disappear after the first few weeks of treatment.
Less common SSRI side effects include nausea, skin rashes, insomnia, headaches and muscle pain. While SSRI medication is considered a first-line treatment for depression, some patients find these symptoms to be adverse enough to warrant stopping this treatment.
SNRI Side Effects
SNRI side effects are similar to SSRIs’ but are usually found to be less severe, this is particularly the case with weight gain and sexual dysfunction. Nausea, dry mouth and headaches rank as some of the more common SNRI side effects, while weight gain, sexual dysfunction, insomnia, and constipation are considered less common SNRI side effects.
TCA Side Effects
TCA side effects are comparatively harsh. In the short-term, TCAs may cause constipation, while its more common side effects include blurred vision, dizziness, and generally higher cardiovascular risk. For these reasons, many find TCAs too adverse to continue.
TMS side effects are normally considered relatively mild, when compared to other treatment options. Side effects between first-generation and Deep TMS slightly vary.
First-Generation TMS
TMS is a non-invasive treatment, and as a result, it avoids complications and side effects that come with invasive procedures or anesthesia. With that said, First-Generation TMS can induce certain reactions. Its more common side effects include headaches, scalp discomfort, lightheadedness, tingling and facial spasms. All these side effects are not long-lasting and normally pass shortly after the session ends.
Deep TMS
As a non-invasive procedure, Deep TMS has been found to be a safe treatment with no significant, adverse, or persistent side effects that are associated. Its most common side effect is a fleeting, localized headache.
A 2007 study published by Clinical Neurophysiology confirmed this finding, concluding that Deep TMS is well-tolerated and does not cause any long-term adverse physical or neurological side effects in patients.
TMS and medication effectiveness may vary, though medication (as well as psychotherapy) are generally accepted as first-line treatments for depression. It should also be noted that either treatment’s efficacy can be enhanced when combined. Deep TMS in particular can be combined with any type of medication as a 2019 study published in the Journal of Psychiatric Research concluded. The study found the treatment to achieve significantly higher remission rates when combined with an antidepressant, as opposed to a depression treatment course that only included medication.
The efficacy of the different medication treatments for depression are rated below. Their rates of success should be considered in regards to each treatment’s tolerability, so that a particularly effective treatment such as TCA treatment could only be considered as a viable option for patients able to withstand some of its more severe side effects.
SSRIs
SSRIs are considered an effective pharmacological treatment for depression. The famed STAR*D study published in 2006 by the American Journal of Psychiatry, echoed the gold standard for SSRI efficacy. The study found that roughly a third of participants reached remission while on the SSRI citalopram, with another 10-15 percent reaching a reduction in symptom severity.
SNRIs
SNRI is another type of medication considered to be an effective treatment option, with approximately 44% of patients achieving remission. SNRI’s higher level of tolerability helps patients continue on with this treatment.
A 2001 study published in the British Journal of Psychiatry reaffirmed this, similarly finding that 45% of patients treated with the SNRI, Effexor, managed to achieve remission. This is compared to 35% of patients treated with an SSRI and 25% of patients who had received a placebo.
Moreover, a meta-analysis study published in Current Medical Research and Opinion in 2006 found SNRIs to have the highest remission and lowest drop-out rates, making SNRIs “clinically superior for treating major depression.”
TCAs
TCA treatment has been found to be highly effective against depression, with certain studies citing a 49% remission rate, while others concluding it to be roughly as effective as SSRIs. TCAs are considered to be particularly efficacious when treating severe depression, though its higher rate of severe side effects cause many patients to discontinue this treatment.
Patients who find the above antidepressants to be tolerable can continue taking them for a long-term remission effect. The chance of relapsing back into depression is inversely related to achieving remission, so that patients who manage to reach remission display lower rates of relapse. The importance of working toward remission is further elucidated when comparing it to a partial response, which only cites a local decrease in symptom severity and frequency. In fact, research has shown that 75% of patients who achieved a positive response from an antidepressant/antidepressant and psychotherapy treatment experienced a depression relapse, while only 25% of patients who achieved remission experienced such a relapse.
TMS has been shown to offer long-term relief from depressive symptoms, though it does necessitate less frequent maintenance treatments. This is the case for both first-generation and Deep TMS.
First-Generation TMS
While First-Generation TMS has been proven to offer patients some symptom relief, it does hold certain limitations. Firstly, the figure 8-coil’s relatively narrow scope only targets a few brain structures at a time, which can cause targeting issues during the procedure. First-Generation TMS also has some difficulty reaching deeper brain structures directly, which can decrease its efficacy as well.
Deep TMS
Deep TMS has repeatedly been proven to alleviate symptoms of depression. An example of this, a 2015 study found that 17.6% of patients experience relapse six months after they finish a Deep TMS treatment course. Conversely, 13.5% of patients undergoing First-Generation TMS had relapsed in the three months following the end of their treatment.
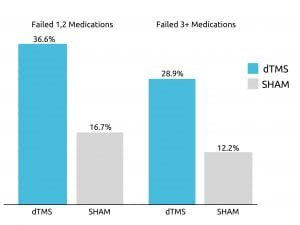
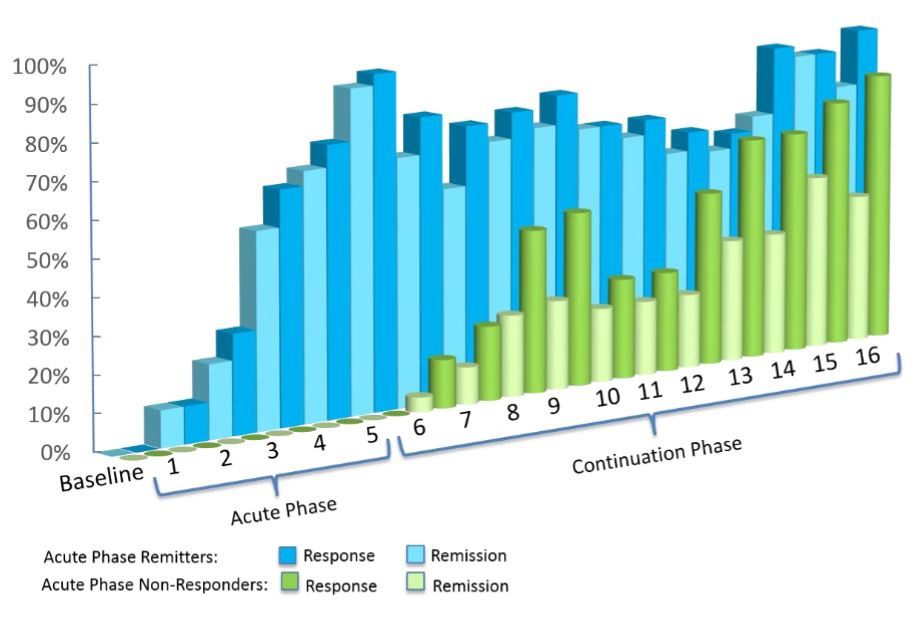
Deep TMS’s effectiveness was presented in a 2015 multicenter sham-controlled study published in World Psychiatry. The study found that approximately one out of three patients with treatment resistant depression managed to achieve remission after four weeks of Deep TMS treatment during the treatment’s acute phase.
The study also found that close to 80% of patients who did not immediately respond to the treatment went on to experience an alleviation of their depressive symptoms during the continuation phase.
In addition to the above lab findings, Deep TMS was discovered to have an even higher success rate among patients in real-life settings, outside of a rigorous clinical study. Specifically, recorded data of over 1000 participants undergoing depression treatment found that roughly 75% achieved a clinical response to Deep TMS, with one out of two patients achieving remission.
It should also be noted that Deep TMS has been shown to increase the chance of remission when combined with an antidepressant. A 2019 study in the Journal of Psychiatric Research reaffirmed this, finding that when combined, Deep TMS and pharmacotherapy therapy resulted in higher rates of remission than pharmacotherapy alone.
When deciding on a treatment course, it is imperative to consult with a licensed medical or mental health professional to examine the different possibilities that are available to you.
Regarding the above option, it can be concluded that both antidepressants and TMS have been shown to offer safe and effective symptom relief from depression. SSRI and SNRI medications are considered a first-line treatment for this condition, and are often considered as an initial treatment option, as is psychotherapy. As a non-invasive form of treatment, TMS can bring about significant and beneficial change in one’s well-being that can be introduced as a standalone treatment or in combination with other forms of therapy, medication included. Patients who battle severe depression, face treatment-resistant depression, or find the side effects of other treatments to be too adverse to continue with them, could greatly benefit from this non-invasive option.
Weighing your mental health treatment options should be done in consultation with a trained health professional, who can offer you advice that can steer you in the direction of the optimal treatment for your specific set of circumstances. Available consultations are offered through such options as your health provider, HMO and local mental health treatment centers.