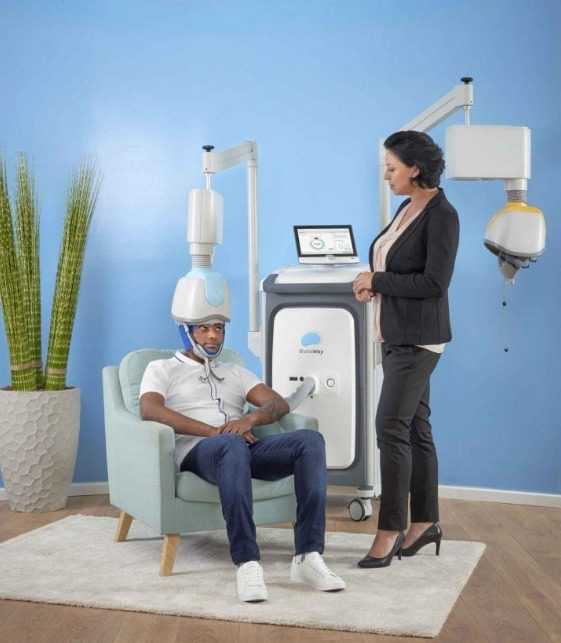
Deep Transcranial Magnetic Stimulation (Deep TMS™) is operated by trained professionals who follow strict regulations to ensure the patient’s safety. As a noninvasive treatment, Deep TMS is a safe, proven and effective therapy course with relatively minor and passing side effects. That said, you should discuss Deep TMS with your doctor to determine if it is right for you and whether any precautions should be taken prior to or during treatment.
Possible Deep TMS Side Effects During and After Treatment
Individuals undergoing Deep TMS treatment may experience mild discomfort during the treatment itself, with some reporting a tapping sensation in the targeted area. Generally speaking, side effects following Deep TMS treatment are normally quite mild.
Possible Deep TMS Side Effects following MDD Treatment
For Major Depressive Disorder (MDD), the most common side effects observed in our multicenter randomized clinical trial during treatment include:
- Site pain (25%).
- Site discomfort (19%).
- Jaw pain (10.2%).
The following side effects were not significantly different in the treatment vs. sham (placebo) groups, and therefore may not be specifically caused by Deep TMS treatment:
- Headaches (47% in treatment group, 36% in sham group). Such headaches tend to get better or go away completely with successive treatments, and can be alleviated using over-the-counter medication.
- Muscle twitching (6% in treatment group, 1% in sham group).
- Back pain (4% in treatment group, 8% in sham group).
- Anxiety (5% in treatment group, 7% in sham group).
- Insomnia (7% in treatment group, 7% in sham group).

Possible Deep TMS Side Effects following OCD Treatment
In a prospective, double-blind, randomized, controlled, multi-center trial on Deep TMS effects on patients with Obsessive-Compulsive Disorder (OCD), the following side effects were observed. No significant differences were seen between the treatment and sham groups, suggesting that these side effects may not be specifically attributable to the magnetic stimulation of the brain involved in Deep TMS treatment.
- Headaches (32% in treatment group, 35% in sham group).
- Anxiety (12% in treatment group, 3% in sham group).
- Jaw pain (8% in treatment group, 1% in sham group).
- Common cold (8% in treatment group, 9% in sham group).
- GI symptoms (8% in treatment group, 0% in sham group).
- Diarrhea (6% in treatment group, 1% in sham group).
- Neck pain, 4% in treatment group, 5% in sham group).
- Fatigue (2% in treatment group, 9% in sham group).
It should also be noted that studies on Deep TMS have shown it to be a safe treatment with no lasting, substantial or systemic side effects, all of which can be caused by medication. Specifically, side effects such as weight gain, dry mouth, sexual problems, or memory effects were not observed in patients following treatment. No longer-term effects were observed during a three-month follow-up.
Deep TMS Safety Concerns
Individuals who fall under the following categories should not undergo Deep TMS Treatment:
- Patients with magnetic metal plates or devices implanted in or around their head (this does not include standard amalgam dental fillings).
- Patients with implanted electronic devices in their body.
- Patients who have undergone a seizure, a medical condition or change in a medical condition that may put them at increased risk of having a seizure.
The safety and effectiveness of BrainsWay’s Deep TMS have not specifically been established in the following patient populations through a controlled clinical trial. Patients should speak with their mental health provider in these cases to assess if Deep TMS is appropriate for them:
- Patients who have a suicide plan or have recently attempted suicide.
- Patients who do not meet DSM criteria for the relevant mental health condition.
- Patients less than 18 years of age or older than 86 years of age.
- Patients with a history of substance abuse.
- Patients with a psychotic disorder, such as schizophrenic disorder, schizoaffective disorder, bipolar disease, or major depression with psychotic features.
- Patients with psychoses or with psychiatric emergencies where a rapid clinical response is needed, such as immediate suicide risk.
- Patients with neurological conditions that include epilepsy, cerebrovascular disease, dementia, increased intracranial pressure, having a history of repetitive or severe head trauma or with primary or secondary tumors in the CNS.
- Patients with metal in or around the head, including metal plates, aneurysm coils, cochlear implants, ocular implants, deep brain stimulation devices, and stents.
- Patients with implants controlled by physiological signals, including pacemakers, implantable cardioverter defibrillators, and vagus nerve stimulators.
- Patients who are pregnant or nursing.
You may also be interested in...