Journal: Journal of Clinical Medicine (2022)
Authors: Gaby S. Pell, Tal Harmelech, Yiftach Roth, Aron Tendler
Background:
Comorbid anxiety is common in patients with major depressive disorder (MDD), and these disorders may share a common underlying pathophysiology. Up to 85% of patients with depression experience significant anxiety symptoms, and comorbid depression occurs in up to 90% of subjects with anxiety disorders.
Objective:
The authors analyzed data from a previous multicenter trial, an independent head-to-head study, and a late-life depression randomized controlled trial to determine if Deep TMS with the H1 Coil is effective in treating comorbid anxiety symptoms in MDD.
Methods:
Data from the three trials using the H1 Coil to treat MDD were evaluated for effectiveness to treat comorbid anxiety. The primary measure was the adjusted Hamilton Depression Rating Scale (HDRS) Anxiety/Somatization (HDRS-A/S) factor score at baseline after 4 weeks of treatment. All patients were treated with H1 Coil using a variant of BrainsWay’s standard high-frequency protocol for depression.
Results:
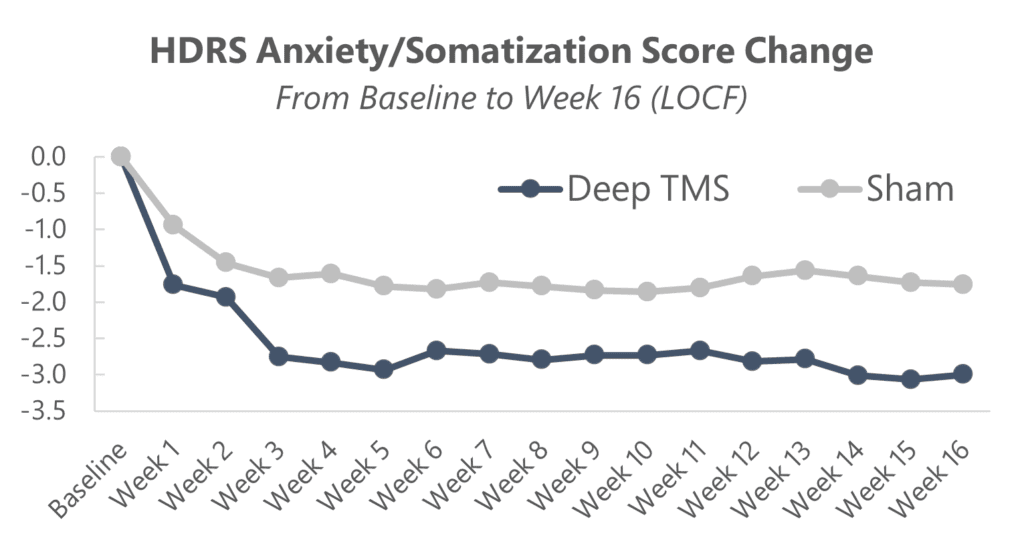
Active Deep TMS compared with the control group in each of the studies showed significantly larger reductions in anxiety scores. These effects were durable for >16 weeks in the pivotal study.
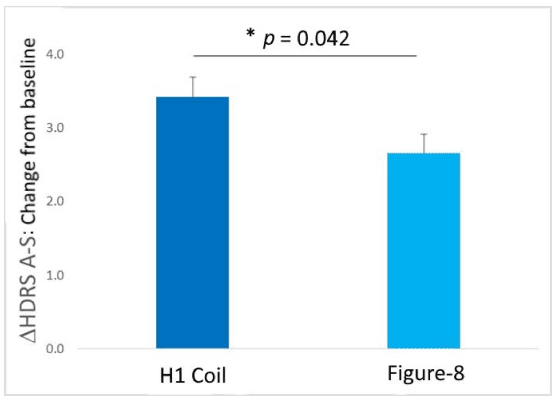
In the independent head-to-head study, a post-hoc direct comparison of the BrainsWay H1 Coil + medication group with the Figure-8 coil* + medication group in the per protocol population demonstrated a statistically significant difference in the reduction in anxiety scores after 4 weeks of treatment in favor of the Brainsway H1 Coil + medication group.
*The Magstim® Rapid² device was used in this study (Magstim Company, Spring Gardens, UK)
Previously reported studies using medication have found that anxiety is a negative predictor of effectiveness. Likewise, a previous study showed that the performance of the Figure-8 coil treatment of MDD was poorer in the subjects with comorbid anxiety disorders.
In contrast, the data from BrainsWay’s pivotal depression study using the H1 Coil, found that reductions in anxiety and depression scores were more pronounced in patients with higher baseline anxiety.
Conclusions:
Deep TMS with the H1 Coil is an effective and robust treatment for anxious depression, a challenging and frequently refractory condition. Using the H1 Coil, outcomes were favorable as compared to anxiolytic medication and first-generation Figure-8 TMS.
Unlike alternative treatments, the outcome does not appear to be adversely affected by high baseline anxiety levels.