To truly understand obsessive-compulsive disorder, we need to learn about how our concept of it has changed and evolved through the years.
Obsessive-compulsive disorder is an anxiety-based mental health disorder that combines distressing thoughts with repetitive behaviors.
OCD obsessions can vary widely, but most often revolve around one or more of the following themes:
OCD compulsions are initially carried out as a calming mechanism, via a repeated action that is initially meant to assuage the anxiety raised by OCD-related thoughts. This can be anything from turning the lights on and off, to an idiosyncratic hand gesture, to repeatedly organizing one’s cabinets. Though at first calming, these ritualistic behavior patterns eventually become compulsive, as with each new enactment they contribute more stress and frustration to the individual who feels compelled to perform them.
It is also worth stressing that it is OCD-induced anxiety, which results from the unyielding thought obsessions and repeated actions, that weighs heaviest on those battling this condition. For this reason, the existence of anxiety is considered a key feature in the definition of this disorder.

Before the mid-1800s, OCD was a little understood condition. Its high levels of anxiety, worrying thoughts and repetitive behavior were explained as symptoms of a number of possible illnesses. Back then, OCD-related symptoms such as obsessive thoughts and compulsive actions were considered part of a number of possible diagnoses, among them: a break from reality, poor blood flow, an intellectual disability or emotional instability.
It was German psychiatrist Carl Westphal who, in 1877, presented the world with a separate definition for OCD-related symptoms. Made even more accurate by his student Robert Thomsen in 1895, Westphal’s definition outlined OCD’s two central features—obsessive thoughts and compulsive behaviors—and highlighted how their presence causes patients increased anxiety. Their efforts resonate to this day, through the way OCD is currently defined and diagnosed.
The father of psychoanalysis, Sigmund Freud saw compulsive OCD behavior as the result of internal conflict. He first referred to OCD as “zwangsneurose,” or “anxiety neurosis,” in 1895, within a paper focusing on anxiety.
According to Freud, some individuals struggle to settle secret, taboo desires within the limitations of social norms and of external reality. These desires are internalized into the unconscious, with its pent-up, frustration eventually manifesting in the uncontrollable urge to carry out illogical actions.
Freud postulated that though these actions offered the patient temporary relief, they also incurred embarrassment, since the patient understood them to be incongruent with normative behavior. Freud’s school of psychoanalysis was the most common form of treatment for OCD well into the mid-20th Century, at which point other forms of treatment became more widely used with this condition.
Interestingly, it was Freud’s choice of words that led to the term we use today: In the UK, “zwangsneurose” was translated as “obsessive neurosis,” while in the US it was translated as “compulsive neurosis.” A compromise between the two was eventually struck, with the term “obsessive-compulsive disorder” emerging as a result.
Following both Westphal’s emphasis on obsessions and compulsions, as well as Freud’s more psychodynamic approach to OCD as a manifestation of taboo desires, official mental health organizations began to take notice of this condition. Specifically, both the American Psychiatric Association’s Diagnostic and Statistical Manual (DSM) and the World Health Organization’s International Classification of Diseases and Illnesses (ICD) included OCD among their recognized mental health disorders, though the condition’s position in relation to other anxiety disorders remained an open debate.

Earlier iterations of the DSM manual featured OCD as part of the anxiety disorders family. And in the current ICD-10, OCD is still featured as part of the “neurotic, stress-related and somatoform disorders” family.
Categorizing OCD under these disorder families made sense, due to its high comorbidity rates with other anxiety-based disorders, as well as the significant damage both OCD and anxiety can cause to one’s life. And so, OCD was seen as another in a row of anxiety disorders, until the publication of the DSM-V.
The DSM’s fifth edition, which was published in 2013, ushered in several new stances in the field of mental health. the manual as a whole moved toward a more developmental approach, detailing which disorders tended to appear before other disorders became apparent; transgender identity was removed and no longer considered a mental disorder; and OCD was given a section of its own, outside of the anxiety disorders family.
There were several reasons that contributed to the extra focus now granted to OCD. First, OCD research has uncovered unique familial, genetic, and neural commonalities among OCD and other OCD-related disorders. In particular, a strong association was found between OCD and abnormalities in brain structures found to be connected to impulse and motor control, as well as self-regulation.
A second contributing factor was the emerging Executive Functioning Hypothesis, which convincingly asserts that OCD evolves out of a disturbance in one’s self-regulatory abilities—while other anxiety-based disorders are more associated with emotional processing.
Together, conclusions from cutting edge research and the Executive Functioning Hypothesis act to reaffirm one another, building the case for increased focus on OCD in light of these developments, as opposed to other disorders that are not yet as well understood.
At present, several treatments have been shown to offer significant symptomatic relief for OCD: Deep TMS, cognitive behavioral therapy (CBT), and SSRI medication.
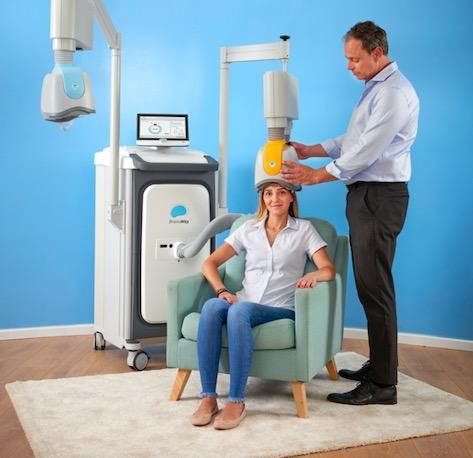
Deep Transcranial Magnetic Stimulation (or Deep TMS) works by utilizing magnetic fields that regulate the neural activity of brain structures such as the anterior cingulate cortex, which has been shown to be associated with OCD. A non-invasive treatment, Deep TMS does not cause any significant or long-lasting side effects or recovery period, and can be combined with any other form of therapy. Due to its safety and efficacy, Deep TMS is the only non-invasive medical device to be FDA-cleared with clinically proven outcome data to treat OCD.
Cognitive behavioral therapy (or CBT) is a form of psychotherapy considered to be a first-line treatment for OCD. This treatment helps the patient identify the thoughts, feelings, behaviors, and physical sensations they associate with their condition. As they learn to acknowledge and respond to triggering stimuli in a way that dismantles their automatic and compulsive OCD responses, patients undergoing CBT gain a better understanding of their condition and solidify their sense of control of it.
Selective serotonin reuptake inhibitor (or SSRI) medication is also considered a first-line treatment for OCD. This group of medications keeps the neurotransmitter serotonin active for a longer period of time, resulting in an elevated mood and a decrease in both anxiety and depression. SSRIs are considered an effective treatment that causes significant OCD symptom relief. That said, it can cause a number of side effects that some patients find to be too adverse to continue treatment. Weight gain, sexual dysfunction and nausea are among SSRIs’ more common side effects.

Perhaps more than anything else, OCD is a lesson in perseverance. Initially a misunderstood condition, it is the unrelenting anxiety that comes with OCD that eventually caused mental health researchers, theorists, and practitioners to pay attention to the suffering experienced by those battling this condition, leading to a more in-depth and comprehensive understanding of it. And as we continue to learn more about OCD, we are able to offer greater care and hope for the individuals who contend with its presence.