Obsessive-compulsive disorder (OCD) is a mental disorder characterized by anxiety-causing thoughts and beliefs, as well as compulsive behaviors intended to calm the induced anxiety. There are currently several OCD treatment options available, offering different methods by which to alleviate the adverse mental health symptoms associated with this condition.
The obsessive thoughts that define OCD intrusively enter the individual’s mind, causing them severe distress. The four main categories of OCD symptoms are: cleanliness and contamination concern (e.g. catching the flu from touching someone else’s plate); worry about disastrous events (e.g. fearing you will get injured every time you leave the house); focusing on neatness, symmetry, counting or “just right” thinking (e.g. repeatedly arranging the markers on a desk so their colors comprise a rainbow); and taboo thoughts (e.g. violent imagery depicting a loved one experiencing a violent act). Beyond the type of obsessive thoughts, OCD is defined by the level of insight, or self-awareness, an individual has into the seriousness of their condition, ranging from good insight to none at all.
The compulsive behavior that defines OCD develops as a coping mechanism intended to assuage the rising anxiety the obsessive thoughts had brought on. However, the resulting behavior ends up amplifying the distress the individual is feeling, causing an escalating cycle that detrimentally affects their physical, social, mental and emotional well-being. Examples of compulsive behaviors related to OCD are varied: they include tediously cleaning the house for fear it is dirty, returning home to make sure all the lights have been turned off, folding and refolding a fitted sheet to get it perfectly flat, or staring at the sun as a ritual meant to “cleanse” the mind from sexual thoughts.
Several treatment options have been determined to offer relief from OCD symptoms. They can be utilized as standalone treatment courses or in combination with one another. In any case, it is recommended you consult with your doctor to find the treatment best suited to your symptoms and needs.
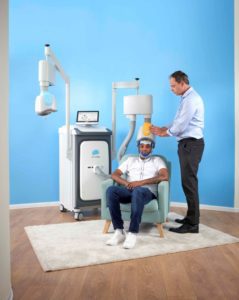
Deep TMS: Deep Transcranial Magnetic Stimulation (Deep TMS™) is a safe, non-invasive treatment that utilizes magnetic fields to regulate the neural activity of brain structures found to be related to OCD. The only non-invasive device FDA-cleared to treat OCD, Deep TMS’s efficacy was confirmed in a 2019 multicenter, sham-controlled study published in the American Journal of Psychiatry, which determined the treatment can significantly alleviate OCD symptoms, particularly for those patients who have not improved from traditional treatment options.
Cognitive Behavioral Therapy: CBT is a branch of psychotherapy that has been found to be effective in treating OCD. The treatment looks at the thoughts, feelings, behaviors and physical reactions that arise from OCD, as the patient is guided to become more familiar with the condition’s symptoms and respond to them in a way that facilitates their dissipation.
Several types of CBT have been found effective for treating OCD, particularly acceptance and commitment therapy (ACT). As part of its treatment course, ACT highlights openness to experience, flexibility in reacting to OCD symptoms, and a commitment to change and wellness.
Exposure and response prevention therapy (ERP) is another form of treatment shown to be effective in alleviating OCD symptoms. The ERP process works by exposing the patient to gradually increasing levels of anxiety, while helping them avoid reacting in a compulsory manner. The end goal in this treatment is to accustom the patient’s brain to the jarring, intrusive OCD-related thoughts so it can begin to respond to them in a more stable and calm manner.
Psychopharmacology: There are several psychiatric medications prescribed for OCD, with antidepressants being FDA-approved to treat it. The approved medications include selective serotonin reuptake inhibitors (SSRIs), and tricyclic antidepressants (TCAs). Psychopharmacology has been known to offer symptom relief to many, though it can also come with various side effects.
Psychodynamic Therapy: Psychodynamics is another form of psychotherapy used to treat OCD. In psychodynamics, the patient and therapist focus on relationships and events that have been central to the patient’s development and have shaped their personality, outlook, and responses to the outside world as well as their emotional landscape. In time, the therapeutic setting can be relied upon to facilitate change and choose new, more adaptive patterns that can help the patient construct a better quality of life.