Obsessive-compulsive disorder (OCD) is currently getting a great deal of attention, due in part to the discovery of specific neural pathways and its focus on everyday, relatable activities such as hand-washing and organization. While OCD certainly deserves to be studied at length, it is actually part of an entire range of fascinating OCD-related disorders, whose symptoms and manifestations are also gaining visibility.
The DSM-V (the fifth edition of the Diagnostic and Statistical Manual of Mental Disorders) characterizes a number of anxiety-based disorders together as “OCD-related disorders.” They include conditions that, like OCD, involve an obsessive thought pattern combined with an unwanted action or ceremony intended to ward off feelings of anxiety.
The OCD-related disorders family includes the following conditions:
Obsessive-compulsive disorder (OCD): An anxiety-based condition that is comprised of obsessive, ruminative thought patterns and compulsive, repetitive behaviors. This disorder essentially acts as an overactive defense mechanism, responding to perceived threats by carrying out repetitive behaviors intended to protect or calm them down. For example, an individual whose OCD manifests itself in obsessive thoughts concerning a disaster harming someone they care about, might initially find it calming to repeatedly turn the lights on and off. Eventually, though, such OCD-related behavior eventually loses its calming effect, becoming a compulsive action that must be performed, which only adds to the individual’s rising anxiety.
The four most common OCD obsessive thought symptoms are disastrous events, symmetry and organization, taboo thoughts, and cleanliness, which has been shown to become incredibly triggering during periods of a widespread health scare.
OCD compulsive behavioral symptoms can vary widely, and include such actions as excessively washing one’s hands, checking and rechecking the oven has been turned off, meticulously organizing all the items in your closet until they are all perfectly aligned, and repeating the same sentence to distract yourself from distressing images of a loved one facing violence.

Body dysmorphic disorder: Characterized by a preoccupation with a perceived or minor physical flaw, body dysmorphic disorder causes the individual to carry out repeated actions (such as looking in the mirror) or mental acts (such as comparing their appearance to those of other people). Many individuals with body dysmorphic disorder pursue repeated plastic surgery to attempt to “rectify” their perceived flaws.
A form of this condition more common in men is muscle dysmorphia, in which the individual is preoccupied by the belief that they are not muscular enough to meet their own standards. To receive this diagnosis, the symptoms of this condition must not be better explained by an eating disorder diagnosis.
Hoarding: An extreme difficulty at the thought of throwing away or parting with physical items, regardless of their actual value, due to a strong perceived need to save them and feelings of distress at the thought of discarding them. Hoarding is different from normal collecting in that the accumulation of possessions clutters and overflows through the rooms of one’s home, negatively affecting the quality of life of those residing in it.
Trichotillomania: Defined by repeatedly pulling out of one’s hair, as well as the continued attempts to refrain from doing so. For many, trichotillomania results in eventual hair loss.

Excoriation: Characterized by picking one’s skin, leading to skin lesions. The skin-picking may be carried out on healthy skin, minor imperfections, acne or marks from previous picking sites.
As opposed to other OCD-related disorders, both trichotillomania and excoriation are not preceded by obsessive thought patterns. There are, however, often preceded by an emotional state involving anxiety or boredom. Following the compulsive hair-pulling or skin-picking characterizations of these two disorders, a sense of gratification, pleasure, or relief may often arise.
Substance/Medication-Induced Obsessive-Compulsive and Related Disorder: This category consists of obsessive-compulsive symptoms that are due to substance intoxication, withdrawal, or relating to medication.
Obsessive-Compulsive and Related Disorder Due to Another Medical Condition: This category includes obsessive-compulsive symptoms linked to OCD and other related disorders that do not amount to an official diagnosis.
The recommended treatments for each OCD-related disorder can vary, mostly in accordance with their individual, defining attributes. That said, cognitive-behavioral therapy (CBT) has generally been found to offer symptom relief for one or more of these conditions.
Individuals facing OCD-related disorders typically respond well to these treatments:
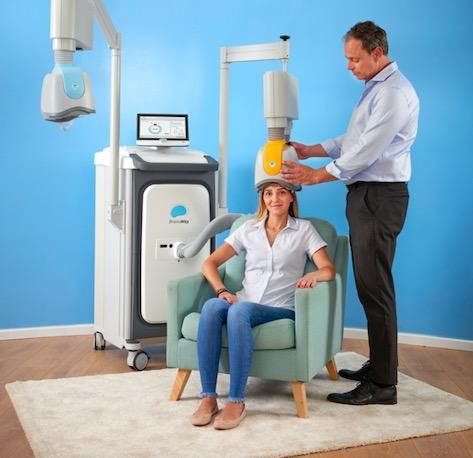
Obsessive-compulsive disorder: Individuals with OCD have been shown to benefit from Deep TMS, CBT and selective serotonin reuptake inhibitor (SSRI) medication. Deep TMS is the only non-invasive medical device to be FDA-cleared with clinically proven outcome data to treat OCD, thanks to published clinical efficacy studies. This patented treatment utilizes magnetic fields to safely and effectively regulate the neural activity of brain structures found to be related to OCD. Deep TMS does not cause any significant or long-lasting side effects, does not necessitate a recovery period, and can be combined with additional treatments, such as psychotherapy or medication.
CBT is a first-line form of psychotherapy that helps patients examine their OCD-related thoughts, feelings, behavior and physical reactions. A goal-oriented approach, CBT gradually familiarizes the patient with elements linked to their anxiety, offering them support as they begin to avoid reacting according to their old, automatic patterns, while replacing them with new, more mindful alternatives. One of the most common forms of CBT for OCD is Exposure and Response Prevention (ERP), which attempts to build tolerance for the obsessive thoughts that plague patients.
SSRI medication is another first-line treatment for OCD (as well as other OCD-related disorders), due to its anxiolytic benefits: SSRIs help keep the neurotransmitter serotonin active for a longer period of time, thereby decreasing one’s anxiety and elevating their mood.
Body dysmorphic disorder: Similarly to OCD, body dysmorphic disorder has also been shown to react well to CBT, by focusing on the patient’s negative self image. Discussing how they view themselves and how they believe others view them helps them face their most painful thoughts within a supportive, therapeutic environment. CBT can also help decrease the patient’s urge to check their reflection, allowing them to focus on other aspects of themselves and their daily routine.
It is also worth noting that while the FDA has yet to approve any medication specifically for body dysmorphic disorder, studies have shown some benefit to SSRI medication when treating this condition.

Hoarding: CBT has also been shown to effectively treat hoarding, through its focus on the excessive collecting and the detrimental beliefs that are part of this disorder. In this case, CBT helps mitigate item acquisition and initiates a sorting process, while also dismantling the unwillingness to part with items and extreme distress that comes with the idea of throwing things out.
Other effective treatments for hoarding include motivational interviewing that incentivizes patients to invest in their own recovery, skill training that teaches patients how to successfully declutter their living environment, and SNRI medication that acts as a mood elevator through both the serotonergic and norepinephrinergic pathways.
Trichotillomania: Another disorder found to respond well to CBT, when treating trichotillomania, CBT experts typically utilize habit reversal to replace the hair-pulling and plucking with a different, non-harmful action. Such actions include squeezing a rubber ball when they feel the urge to tug at their hair, exercise, take a bath and more. Keeping a diary is also encouraged, as a means of keeping track of the treatment’s challenges and progression.
Additionally, acceptance and commitment therapy, or ACT, has also been shown to benefit patients with trichotillomania, by developing their cognitive flexibility and perseverance when faced with the anxiety that comes with this condition.
Excoriation: Patients with this skin-picking disorder typically benefit from psychotherapy, and specifically from CBT and a focus on habit reversal. CBT works by focusing on psychoeducation regarding this lesser-known condition, cognitive restructuring concerning the patient’s urge to skin pick, and building their self-efficacy around their ability to avoid this behavior.
Habit reversal works similarly with excoriation as it does with trichotillomania, with the treatment working to replace the detrimental form of behavior with a non-harmful alternative, to alleviate stress and build a new cognitive connection between stressful urges and a calming, repetitive action.
With researchers, therapists and society at large raising awareness for OCD-related disorders, more of those battling these conditions are able to receive the treatments they need and the understanding and empathy they deserve, in their journey toward a better quality of life.